A 50 year old male with abdominal distention and pain abdomen
This is an a online e log book to discuss our patient de-identified health data shared after taking his / her / guardians signed informed consent. Here we discuss our individual patients problems through series of inputs from available global online community of experts with an aim to solve those patients clinical problem with collective current best evident based input.
This E blog also reflects my patient centered online learning portfolio and your valuable inputs on the comment box is welcome.
I have been given this case to solve in an attempt to understand the topic of " patient clinical data analysis" to develop my competency in reading and comprehending clinical data including history, clinical findings, investigations and come up with diagnosis and treatment plan
The patient/ attender was informed the purpose of the information being acquired. An informed consent was taken from patient/ attender and there is omission of information that was requested to be omitted.
CONSENT WAS GIVEN BY BOTH PATIENT AND ATTENDERS
Chief complaints :
A 50 year old male a government revenue employee by occupation came with a Che if complaints of
★ abdominal distention and pain abdomen since 1 week
★shortness of breath since 1 week
★ b/l lower limb sweeping since 5 days
★decreased urine output and yellowish discoloration of urine since 5 days
★ loss of appatite since 5 days
History of present illness :
Patient was apparently asymptomatic one week back then he noticed abdomeninal distention which was diffuse associated with abdominal pain( squeezing type ) not associated with vomotings , loose stools , fever . aggravated with food intake .
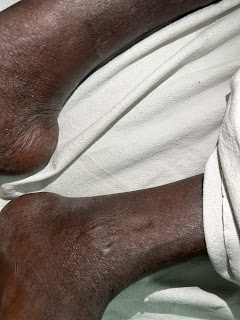
Complaints of bilateral pedal edema which is pitting type gradually progressive, extending from ankle to knee joint
C/o decreased urine output and yellowish discolouration of urine since 5 days not associated with fever with chills and burning miturition , frothing of urine
No h/o chest pain , palpitations , excessive sweating .
Complaints of shortness of breath with grade II which is decreased in supine position
No H/o hematemisis , melena
He is a government revenue employee who wakes up at 6 am do his daily routine and hurriedly goes to his work mostly he skips his breakfast . up to 2 pm he doesn't have time he is busy with his respective work at 2 pm he takes his lunch and comes to home by 6 to 6:30 pm the he goes to drink alcohol( whiskey 180 ml ) this was his daily routine since 12 years .
3 years back the patient was admitted in hospital for 15 days he was diagnosed with dengue ( ? Coma)
2 years back he had jaundice for which he had a 2 PRBC transfusions
Recently 20 days back he is having decreased vision so he went to checkup and diagnoses with cataract , he was adviced to stop alcohol so he stopped alcohol 15 days back
Past history
Not a known case of HTN , Diabetes , asthma , TB , epilepsy , CAD ,CVD , thyroid diseases
H/o appendicectomy 17 yes back
Personal history
He takes mixed diet
Appetite : decreased since 5 days
Sleep : adequate
Addictions :Alcoholic since 12 years,he used drink 180 ml of whiskey twice a week but from last 6 years he began drinking 180 ml of whiskey daily, but stopped drinking 15 days ago.
No h/o smoking
Family history
Not significant
GENERAL EXAMINATION
Patient was conscious,coherent cooperative poorly build and nourished
Pallor : present
Icterus: present
clubbing: absent
cyanosis: absent
Lymphadenopathy: absent
Edema : present
Cataract :
VITALS:
On 2/1/23
Temp : afebrile
BP : 110/90 mmHg
Pulse : 90 bpm
RR : 22cpm
Spo2 : 98%
On 3/1/23
Temp: afebrile
BP : 110/70 mmHg supine position
Pulse : 92 bpm
RR : 20cpm
Grbs : 101 mg /dl
Systemic examination
Per abdomen :
On Inspection :
Abdomen is distended
Visible veins are seen
Flanks are full
A rash is seen in the region xiphoid process to left
Umbilicus : flat
An appendecectomy scar is present in right iliac fossa
Palpation :
No local raise of temperature
Abdomen is tense
abdominal girth : 93 cms
Mild tenderness over right hypochondrium
Liver and spleen are not palpable
On percussion
A dull note is heard
On auscultation
Decreased bowel sounds are heard
Respiratory system
On inspection :
Shape of chest is normal
Looks like symmetrically expanding
No scars and sinuses
Trachea is central
On palpation :
no local raise of temperature or tenderness
All inspectory findings were confirmed
Chest is symmetrically expanding On both sides
On percussion
Purssion note is same on both sides
On auscultation :
Bilateral air entry was present
Crepitus was heard in the right and left inframammary, supra mammary , infra axillary areas
CVS :
S1 S 2 heard apex beat felt at 5th inter coastal space lateral to mid clavicular line no murmors
CNS examination
HIGHER MENTAL FUNCTIONS:
Conscious, coherent, cooperative
Appearence and behaviour:
Emotionally stable
Recent,immediate, remote memory intact
Speech: comprehension normal, fluency normal
CRANIAL NERVE:
All cranial nerves functions intact
SENSORY FUNCTIONS
SPINOTHALAMIC TRACT
Pain , temperature ,presure- intact in all limbs
Posterior column:
Fine touch, vibration and proprioception are intact
MOTOR SYSTEM :
Right Left
Bulk:
Inspection. N. N
Palpation. N. N
Tone:
UL. N. N
LL. N. N
REFLEXES :
B T S K A P
R + + + + + Flexor
L + + + + + Flexor
CEREBELLUM:
Finger nose Incoordination - No
Knee heel incoordination - No
DIAGNOSIS
Decomoensated liver disease 2° to pancreatitis 2° to alcohol abuse
INVESTIGATIONS
TREATMENT :
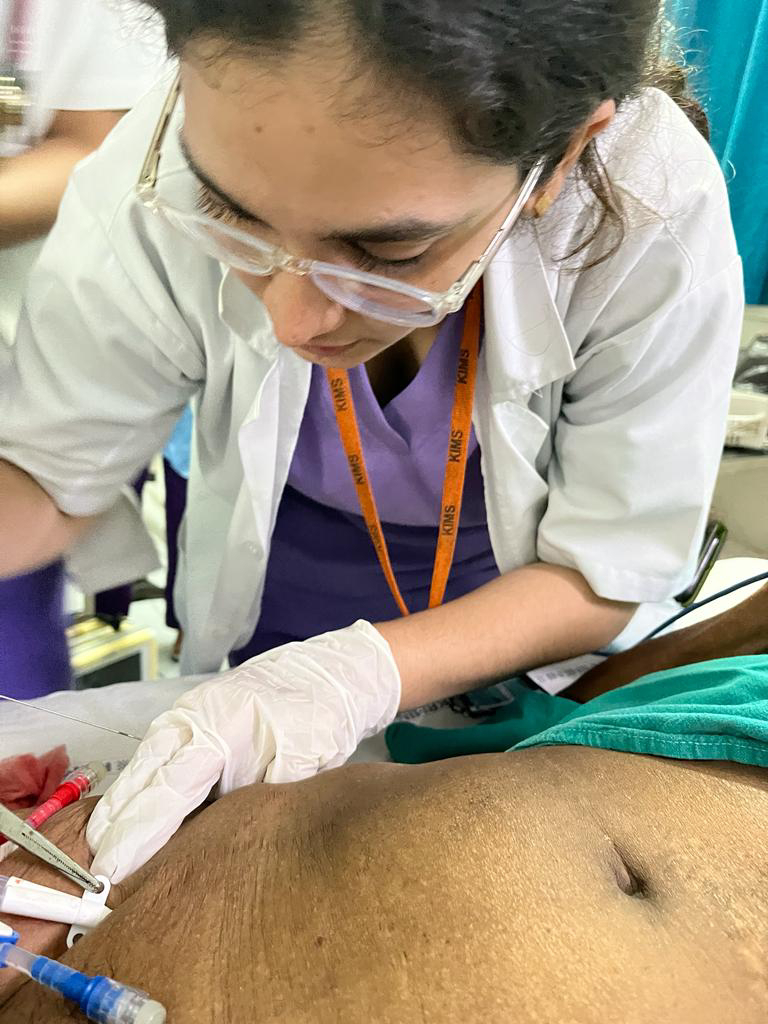
Ascitic tap was done but no fluid was drained
• Fluid restriction less than 1.5 L /day
• Salt restriction less than 2g/day
• Inj Lasix 40mg IV BD
• Syp lactulose 30ml PO
• Maintain 2-3 times passage of stools
• TAB Gabapentin 100mg PO BD
• Inj Monocef
• TAB Aldactone 50 mg PO OD


























Comments
Post a Comment